Sedation dentistry describes a range of techniques used to help children feel calm and safe during dental care. For many families, routine visits are simple and stress-free; for others—especially young children, those with strong gag reflexes, sensory sensitivities, or prior negative experiences—sedation can make necessary treatment possible without trauma. The goal is not to remove awareness entirely in every case, but to tailor comfort to each child’s needs so care can be completed efficiently and compassionately.
Choosing the right level of sedation starts with a careful evaluation of the child’s medical history, anxiety level, developmental stage, and the scope of planned treatment. We balance clinical objectives with the child’s emotional well-being, favoring the least invasive option that will allow safe, cooperative care. Parents are partners in that decision-making process: clear explanations and realistic expectations help families feel prepared and confident before their appointment.
Modern pediatric sedation is supported by rigorous training, standardized protocols, and continuous monitoring. Techniques range from nitrous oxide, which offers mild calming effects, to oral medications that induce a twilight-like state, and, for specific situations, deeper sedation administered intravenously under the supervision of an anesthesiology professional. Each approach has advantages—and the team’s priority is always the child’s safety and comfort throughout the experience.
When sedation is recommended, clinicians discuss the plan in plain language: what will happen, why it’s needed, how you should prepare, and what to expect afterward. This transparent approach reduces surprises for both child and caregiver and helps build trust in the care process. With thoughtful preparation and skilled providers, sedation can transform a previously stressful visit into a manageable and even positive step in a child’s oral health journey.
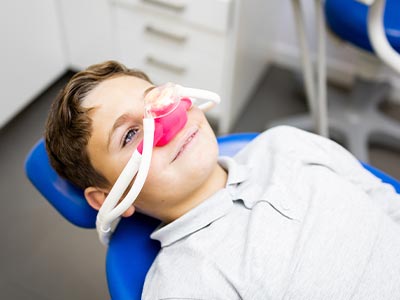
Nitrous oxide—commonly called “laughing gas”—is a safe, well-established option for minimal sedation in pediatric dentistry. Delivered through a small mask that fits over the child’s nose, nitrous oxide produces a gentle sense of relaxation within minutes and wears off quickly once the mask is removed. Its rapid onset and recovery make it particularly useful for routine restorative care, simple extractions, or for children who are nervous but otherwise cooperative.
One of the primary benefits of nitrous oxide is its controllability. The dental team can adjust the level of sedation during treatment, increasing or decreasing the calming effect as needed. Because the gas is eliminated through normal breathing, most children are alert and able to return to regular activities shortly after the appointment. This makes nitrous oxide a convenient and efficient choice for parents and clinicians alike.
Beyond reducing anxiety, nitrous oxide has mild analgesic properties that can improve comfort during procedures. It is typically well tolerated and carries a low risk profile when administered by trained personnel. Still, it is not the right solution for every child—those with certain respiratory issues or nasal obstructions may need alternative approaches—and a thorough pre-visit assessment helps identify the best method for each patient.
Parents often appreciate the predictable nature of nitrous oxide: the dental team can explain its effects in advance, demonstrate the mask, and let the child acclimate before any treatment begins. That familiarity can turn an unfamiliar clinic experience into something manageable, and for many families, nitrous oxide is the first step toward building confidence with dental care.
Oral conscious sedation refers to medication taken by mouth prior to the appointment to reduce anxiety and promote a drowsy, relaxed state. Often described as a “twilight” level of sedation, this approach helps children who are highly anxious or have difficulty cooperating for the entire duration of treatment. Unlike deep anesthesia, patients under oral sedation typically remain responsive to gentle stimulation and can follow simple instructions when necessary.
Oral sedation is particularly useful when multiple procedures are required in a single visit or when a child’s anxiety would otherwise prevent completion of treatment. The medication is carefully dosed based on age, weight, and medical history, and families receive clear instructions on timing and pre-appointment care to ensure effectiveness and safety. Because the sedative effects persist into the recovery period, caregivers should plan to provide close supervision and avoid driving or complex activities for the remainder of the day.
Communication before the visit is essential: providers review current medications, recent illnesses, and any sleep or developmental concerns that could affect the sedation plan. During the appointment, the team maintains continuous monitoring and is prepared to modify the plan if a child is more or less sedated than expected. That adaptability helps ensure that the dental work is completed without unnecessary interruptions while preserving the child’s stability and comfort.
For many families, oral conscious sedation offers a practical middle ground—stronger calming effects than nitrous oxide, with fewer logistical demands than general anesthesia. When administered with careful planning and professional oversight, it allows children to undergo necessary care with minimal psychological stress and a lower likelihood of needing repeat appointments.
There are occasions when deeper sedation or general anesthesia is the most appropriate and humane choice—particularly for very young children, those with severe anxiety or sensory challenges, or cases requiring extensive treatment that cannot be safely completed under lighter sedation. In such situations, IV sedation or general anesthesia produces a controlled, reversible state of unconsciousness so the dental team can work efficiently and safely while the patient remains fully comfortable.
When deeper sedation is required, care is coordinated with a dental anesthesiologist or an appropriately trained anesthesia provider who brings specialized expertise to in-office procedures. These visits involve more extensive preoperative planning, including medical clearance when indicated, specific fasting instructions, and a detailed discussion of risks and benefits with the child’s caregiver. Because of the additional resources and personnel involved, these cases are scheduled with extra time and careful logistical planning.
Whether a child receives IV sedation or general anesthesia, the emphasis is on rigorous monitoring and recovery protocols. The anesthesia team uses advanced equipment to continuously track airway status, oxygenation, heart rate, and blood pressure. After the procedure, patients move to a recovery area until they meet safety criteria for discharge, and caregivers receive clear post-operative instructions to support a smooth recovery at home.
Safety is the cornerstone of pediatric sedation. Every sedation option is accompanied by standardized monitoring and emergency preparedness: trained staff, appropriate resuscitation equipment, and protocols tailored to children’s specific needs. Continuous observation during and after sedation helps ensure any changes in a child’s condition are recognized and addressed promptly. The goal is predictable, safe care that minimizes risk while maximizing comfort.
Preparation is a shared responsibility between the dental team and caregivers. Before any sedated appointment, clinicians collect a detailed health history, review current medications, and explain fasting and medication guidelines. Following these instructions closely reduces the risk of complications and supports a smoother anesthesia process. On the day of the procedure, arriving on time and with the necessary paperwork helps everyone stay on schedule and focused on the child’s well-being.
Aftercare is equally important. Children recovering from sedatives need quiet, supervised rest and gradual return to normal activity, according to the provider’s recommendations. The dental team will provide clear, written post-operative guidance so parents know what signs to watch for and when to seek further care. With appropriate preparation and follow-up, sedation can be a safe, effective tool that enables essential dental treatment without undue stress.
At Happy Campers Pediatric Dentistry, our approach to sedation is conservative, family-centered, and safety-first. We tailor each plan to the child in front of us—choosing the gentlest effective option and explaining every step so caregivers feel informed and reassured. If you’re considering sedation for your child or want to learn which option may be best, please contact us for more information; our team is happy to discuss the process and help you plan a calm, successful visit.
Sedation dentistry uses a range of methods to help children remain calm and comfortable during dental treatment while allowing clinicians to complete needed care safely and efficiently. Techniques vary from minimal, short-acting options to deeper, medically supervised sedation depending on the child’s needs and the complexity of the procedure. The primary goal is to reduce fear and stress while preserving the child’s ability to cooperate as appropriate for the chosen method.
Clinicians select the least invasive approach that will achieve the clinical objectives and protect the child’s emotional well-being, and families are included in the decision process. Pre-visit evaluation, clear communication, and a calm environment help ensure that sedation supports a positive overall experience. When properly planned and monitored, sedation can transform a difficult visit into one that is manageable and less traumatic for both child and caregiver.
Determining the appropriate level of sedation begins with a comprehensive assessment that includes the child’s medical history, age, weight, anxiety level, developmental considerations, and the scope of the planned dental work. The dental team evaluates potential risks and benefits and favors options that provide effective comfort with the lowest necessary depth of sedation. Parental involvement and informed discussion of expectations are central to choosing a safe, effective plan.
Clinicians also consider practical factors such as whether multiple procedures will be completed in one visit and whether the child has respiratory or other medical conditions that affect sedation choices. For deeper sedation or general anesthesia, coordination with an anesthesia provider and additional preoperative planning are required. Throughout the process, flexibility is important: the team monitors the child’s response and adjusts the approach as needed to maintain safety and comfort.
Nitrous oxide, often called laughing gas, is a commonly used minimal sedation option in pediatric dentistry that produces a gentle sense of relaxation within minutes and dissipates quickly after the mask is removed. It is delivered through a nasal mask and can be adjusted during treatment to reach the desired calming effect while preserving the child’s ability to respond to instructions. Because it is eliminated through breathing, recovery is rapid and most children can resume normal activities shortly after the appointment.
When administered by trained staff under established protocols, nitrous oxide has a favorable safety profile and provides mild analgesia in addition to anxiety reduction. It is not appropriate for every patient; children with certain respiratory problems or nasal obstructions may require alternative methods. A pre-visit assessment helps identify the best and safest option for each child.
Oral conscious sedation involves one or more medications taken by mouth before the appointment to produce a drowsy, twilight-like state that reduces anxiety and promotes cooperation during dental treatment. Dosages are carefully calculated based on age, weight, and medical history, and caregivers receive specific instructions on timing, fasting, and medication interactions to ensure safety and effectiveness. Children under oral sedation generally remain responsive to gentle stimulation and can follow simple directions when needed.
Because the sedative effects last into the recovery period, caregivers must plan to supervise the child closely after the appointment and avoid activities such as driving or vigorous exercise for the remainder of the day. The dental team monitors the child continuously during the visit and is prepared to adjust care if the level of sedation differs from expectations. Clear communication and adherence to pre- and post-visit instructions are key to a smooth experience.
IV sedation or general anesthesia is recommended when lighter methods are unlikely to provide adequate comfort or safety, such as for very young children, those with severe dental anxiety, significant sensory processing differences, or when extensive treatment must be completed in a single visit. These approaches produce a deeper, controlled state of unconsciousness so the dental team can perform complex procedures without distress to the child. Because they carry greater physiological effects, deeper sedation requires coordination with a qualified anesthesia provider and more extensive preoperative planning.
Visits involving IV or general anesthesia include additional safety steps: medical clearance when indicated, specific fasting instructions, and dedicated monitoring and recovery resources. The anesthesia provider and dental team use advanced equipment to continuously track airway, oxygenation, heart rate, and blood pressure throughout the procedure. Afterward, patients remain under observation in a recovery area until they meet established criteria for safe discharge to a responsible caregiver.
Safety is the highest priority for any sedated dental visit and is ensured through staff training, standardized protocols, and continuous physiologic monitoring tailored to pediatric patients. Trained personnel maintain vigilance throughout the procedure using equipment to track oxygen saturation, heart rate, blood pressure, and respiratory status, and emergency equipment and medications are readily available. Regular drills, clear role assignments, and adherence to evidence-based guidelines help the team respond promptly to any unexpected changes.
Pre-visit screening and thorough medical review reduce the likelihood of complications by identifying conditions that affect sedation choices or require additional precautions. In cases requiring deeper sedation or anesthesia, a credentialed anesthesia provider is involved and the visit includes additional planning and recovery time. Transparent communication with caregivers about the monitoring plan and safety measures helps build confidence and ensures everyone understands what to expect.
Preparation typically involves following fasting and medication instructions provided by the dental team, reviewing the child’s current medications and recent health changes, and arriving on time with any required forms or documentation. Caregivers should plan to provide a calm arrival, bring a favorite comfort item if allowed, and arrange for responsible adult supervision and transportation home after the appointment. Clear pre-visit guidance helps minimize the risk of complications and supports a smooth sedation experience.
Discussing the visit in age-appropriate language and avoiding frightening phrases can reduce anxiety before the appointment, and the dental team will explain what to expect in plain terms. For oral sedation, timing of medication is important; for IV or general anesthesia, more specific fasting rules and preoperative steps will be given. Following all instructions closely is an essential part of ensuring safety and a successful outcome.
After a sedated appointment, children are monitored in a recovery area until they meet safety criteria for discharge, including stable breathing, alertness appropriate to the method used, and normal vital signs. Recovery time varies by the type of sedation: nitrous oxide typically wears off quickly, while oral or IV sedation produces drowsiness that may last several hours. The dental team provides clear, written aftercare instructions outlining activity restrictions, signs to watch for, and guidelines for pain management or medication if needed.
Caregivers should plan quiet, supervised rest for the remainder of the day and avoid allowing the child to engage in strenuous activity, swimming, or return to school until the provider gives clearance. If any unexpected symptoms arise—such as difficulty breathing, persistent vomiting, or prolonged unresponsiveness—caregivers should contact the dental office or emergency services immediately. Following the provided aftercare plan supports a smooth recovery and reduces the likelihood of complications.
While sedation is generally safe when delivered by trained professionals following established protocols, no medical intervention is without risk; common short-term effects can include drowsiness, nausea, or mild respiratory changes that are typically transient. The likelihood of adverse events is minimized by careful patient selection, dose adjustments based on age and weight, thorough pre-visit screening, and continuous monitoring during and after the procedure. The team also prepares for rare emergencies with appropriate equipment and training.
Serious complications are uncommon but may include respiratory depression or allergic reactions, which is why communication about the child’s medical history, current medications, and previous anesthesia experiences is essential. Informed consent and a clear explanation of risks, benefits, and alternatives help families make well-informed decisions. Ongoing quality assurance and adherence to pediatric sedation guidelines further reduce risk and promote consistent, safe care.
Talking to a child about sedation in calm, age-appropriate terms helps reduce fear and sets realistic expectations: describe the visit as a way to help teeth stay healthy, explain that the team will help them feel sleepy or relaxed, and avoid using scary words such as "pain" or "needle" when unnecessary. Role-playing the visit with a favorite toy, reading simple books about doctor or dentist visits, and scheduling a pre-visit office tour if available can make the environment feel familiar. Honesty balanced with reassurance builds trust and helps the child feel prepared.
Encourage questions and model a relaxed attitude, since children often take cues from caregivers’ emotions. The dental team can offer strategies tailored to the child’s age and temperament, such as breathing exercises, distraction techniques, or a demonstration of equipment to demystify the process. Combining parental support with professional guidance helps the child face the appointment with greater confidence and reduces the need for deeper sedation when appropriate.
Quick Links