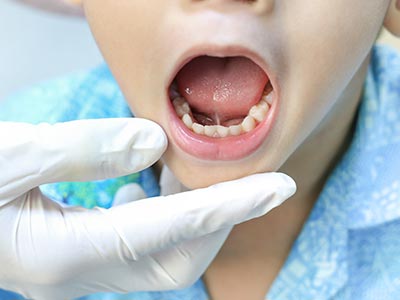
Tongue and lip ties occur when the small bands of tissue that connect the tongue or upper lip to the mouth (called frenula) limit normal movement. In many children those bands are thin and flexible, but in some infants the tissue is tight, thick, or positioned in a way that restricts motion. That restriction can interfere with a child’s ability to latch, swallow, or make certain oral movements that support feeding and early speech development.
These conditions are present at birth and can range from barely noticeable to functionally limiting. Not every tight frenulum requires intervention — many children adapt well and show no lasting problems — but when ties create feeding difficulty, pain, or delayed milestones, they become clinically significant. Early recognition helps families and clinicians decide whether monitoring, therapy, or a release procedure is the best next step.
Awareness is helpful because ties can show up in a variety of ways beyond feeding. They may affect bottle or breast feeding, tooth alignment as permanent teeth arrive, and speech patterns later in childhood. A careful, individualized assessment ensures that decisions about treatment focus on function and comfort rather than appearance alone.
When a tie interferes with typical tongue or lip movement, the most immediate and noticeable effects often involve feeding. Infants may struggle to form a secure latch at the breast, work hard while feeding, or take unusually long to feed. These challenges can lead to frequent waking for additional feeds and parental worry about weight gain and nutrition.
Mothers may also experience symptoms related to feeding mechanics. Pain during nursing, recurring plugged ducts, and episodes of mastitis can result from a shallow or inefficient latch. In some situations, milk supply may be affected because feeding is less effective and more stressful for both mother and baby.
Infant signs to watch for include poor weight gain, visible clicking or slipping while feeding, frequent spit-up or reflux-like symptoms, excessive drooling, and fussiness around feeding times. Some babies show persistent gas or prolonged nursing sessions because they cannot transfer milk efficiently. While these signs do not automatically confirm a tie, they are common reasons families seek evaluation.
Because symptoms overlap with other conditions, clinicians often consider ties alongside other possible causes. Collaborating with pediatricians, lactation consultants, and speech or feeding therapists helps create a complete picture so that any recommended treatment targets the underlying functional problem.
Assessment begins with a careful history and a gentle oral exam focused on how the tissue affects movement and function. We observe feeding when possible, ask about specific symptoms, and may invite input from lactation specialists or pediatric providers already involved in the child’s care. The goal is to determine whether limited mobility is the primary cause of the feeding or comfort issues families are seeing.
Not all ties require a release. For some infants, supportive strategies such as positioning adjustments, targeted breastfeeding techniques, or feeding therapy are sufficient. When conservative measures don’t produce the needed improvement, a release procedure may be recommended to restore range of motion and improve function.
We offer complimentary consultations so parents can ask questions and see how a recommended plan fits their child’s needs. During these visits we explain the rationale for any proposed procedure, outline what to expect during and after the appointment, and coordinate care with other professionals to ensure a consistent, supportive approach.
A diode laser release is a targeted, minimally invasive procedure used to release tight frenula under controlled conditions. The laser allows the clinician to make precise adjustments to the tissue with minimal bleeding and a focused application that limits trauma to surrounding structures. For many infants the process is brief and well tolerated, which is why laser techniques are commonly recommended for this age group.
Before the procedure, the team reviews the child’s history and confirms that the proposed treatment is appropriate. Comfort measures may include topical anesthetic, sucrose, swaddling, or other age-appropriate supports to reduce movement and anxiety. The release itself typically takes only a few minutes, and the laser’s cauterizing effect reduces the need for sutures.
Safety and gentle care are priorities. Throughout the appointment the team monitors the infant and uses techniques to keep the experience calm for both child and family. Because every child is different, we tailor our approach to provide the least invasive, most effective care possible while explaining each step so parents know what to expect.
Potential risks are small but will be discussed during the consultation. These conversations cover immediate aftercare, signs of normal healing versus unexpected changes, and the anticipated timeline for improvement in feeding or comfort after a release.
Healing after a release is usually rapid, but active aftercare helps optimize results. Families are often shown simple oral stretches and positioning techniques to prevent reattachment and promote full range of motion. These exercises are brief and are typically done several times a day for a short period during the initial healing phase.
Improvements in feeding may be immediate for some infants and gradual for others. Even when the physical restriction is removed, babies who have adapted to inefficient feeding patterns sometimes need support to relearn an efficient latch. Coordination with lactation consultants or feeding therapists can be an important part of the recovery plan to ensure stronger, more comfortable feeding sessions.
Follow-up visits let the clinician assess healing, confirm improved mobility, and address any lingering concerns. Most children experience meaningful benefits from a successful release, including reduced pain for nursing caregivers and more effective feeding for the infant. The long-term outlook is favorable when the procedure is part of a coordinated plan that includes appropriate follow-up care.
If questions arise during recovery, families are encouraged to contact their care team promptly. Early communication helps address routine concerns and prevents small issues from becoming more significant.
Selecting a team that listens, evaluates function carefully, and offers coordinated follow-up is important. At Happy Campers Pediatric Dentistry we emphasize a child-centered approach that blends clinical experience with practical, family-focused support. Our goal is to restore natural movement when a tie is clearly causing problems and to provide clear guidance for what happens before, during, and after a release.
We work closely with pediatricians, lactation consultants, and therapists to create a consistent plan tailored to each child. That coordination helps ensure that any recommended release is part of a broader strategy to improve feeding, comfort, and development rather than a standalone intervention.
Parents who pursue a consultation can expect respectful, evidence-informed advice and a transparent discussion of alternatives. We prioritize the least invasive option that meets the child’s needs and provide the education families need to support recovery at home.
In summary, tongue and lip ties can meaningfully affect feeding, comfort, and early development for some infants. A careful assessment clarifies whether a tie is the primary cause of symptoms and whether a release is the best choice. If you’d like to learn more about evaluation and treatment, please contact us for additional information and to schedule a consultation.
Tongue and lip ties occur when the thin bands of tissue called frenula limit normal movement of the tongue or upper lip, and these differences are present at birth. In some infants the tissue is thin and flexible, while in others it is short, thick, or attached in a way that interferes with motion needed for feeding and early oral development. Identifying a tie is about function rather than appearance, because limited mobility can affect feeding mechanics, dental development, and speech milestones.
Not every tight frenulum requires treatment, since many infants adapt without lasting problems, but ties that cause pain, inefficient feeding, or delayed milestones are clinically significant. Early recognition allows families and clinicians to choose monitoring, therapy, or a release procedure based on documented functional concerns. A careful, individualized assessment focuses on restoring comfortable, effective movement rather than correcting appearance alone.
Ties can change the way an infant forms a latch, transfers milk, and swallows, which often shows up as long, tiring feeds, visible clicking, or poor weight gain in some babies. Nursing parents may report nipple pain, recurring plugged ducts, or mastitis linked to a shallow or inefficient latch, and bottle feeding can be equally affected when milk transfer is compromised. These feeding challenges can also lead to increased gas, frequent spit-up, and fussiness during or after feeds.
Because feeding symptoms overlap with other conditions, a thorough evaluation often involves observation of feeds and input from lactation consultants or pediatric providers. Treatment decisions are based on whether restricted mobility is the primary cause of the feeding problem and whether conservative measures improve function. When conservative strategies do not resolve feeding difficulties, a release may be considered to restore range of motion and support more efficient feeding.
Evaluation begins with a detailed history and a gentle oral exam that focuses on how tissue restricts movement and affects function rather than just appearance. Observing feeding when possible, asking targeted questions about symptoms, and documenting feeding efficiency help clinicians determine the role a tie plays in a child’s difficulties. Because feeding issues can be multifactorial, collaboration with pediatricians, lactation consultants, and feeding or speech therapists is often essential to create a complete picture.
The office of Happy Campers Pediatric Dentistry offers complimentary consultations to review concerns, explain possible next steps, and coordinate care with other professionals already involved in the child’s care. These visits are intended to provide families with clear, evidence-informed options and to identify whether monitoring, therapy, or a release is the most appropriate intervention. A team-based approach ensures that any recommended procedure is part of a broader plan to improve feeding and comfort.
A release is typically recommended when limited frenulum mobility is clearly linked to persistent functional problems such as painful nursing, poor weight gain, or significant speech and dental concerns that do not improve with conservative care. Many infants respond well to positioning changes, feeding technique adjustments, or targeted feeding therapy, so clinicians often try these measures first when feasible. The decision to proceed with a release is always based on documented functional benefit rather than appearance alone.
Clinicians will consider the severity of symptoms, the child’s age, and response to conservative measures when recommending a release, and they will explain alternative options during the consultation. When a release is chosen, it is coordinated with the rest of the care team to ensure feeding support before and after the procedure. Follow-up and therapy are commonly part of the plan to help infants relearn efficient movement after a release.
A diode laser release is a focused, minimally invasive procedure that precisey releases tight frenula while minimizing bleeding and trauma to surrounding tissue. Comfort measures such as topical anesthetic, sucrose, swaddling, and age-appropriate soothing techniques are commonly used to keep the infant calm and still, and the actual laser release often takes only a few minutes. Because the laser cauterizes as it works, sutures are frequently unnecessary and recovery is typically rapid.
Safety and gentle care are priorities throughout the appointment, with continuous monitoring of the infant and clear explanations for the family about each step. Potential risks and immediate aftercare instructions are reviewed during the consultation so parents know what to expect. The brief nature of the procedure and its targeted approach make it a commonly chosen option for infants when a release is indicated.
Healing after a release is usually quick, but active aftercare helps achieve the best results and reduces the chance of reattachment. Families are typically taught simple oral stretches and positioning techniques to be performed several times daily for a short period, and these exercises promote full range of motion and healthy scar formation. Proper postprocedure care also includes monitoring for signs of normal healing versus unexpected issues and maintaining close communication with the care team.
Because babies who have adapted to inefficient feeding patterns may need help relearning an effective latch, coordinated feeding support from lactation consultants or feeding therapists is often recommended. Follow-up visits allow clinicians to assess mobility, confirm healing, and address any lingering concerns. Prompt questions or concerns during recovery should be reported to the care team to prevent small issues from becoming more significant.
Potential risks of a release are generally small but can include bleeding, infection, or incomplete release that may require additional follow-up. Laser techniques reduce bleeding and tissue trauma, but families should still be informed about signs of normal healing and indicators that warrant prompt reassessment. Clinicians discuss these possibilities during the consultation so parents understand both typical recovery and uncommon complications.
Longer term concerns such as reattachment are minimized with proper aftercare and stretches, while collaboration with therapists can help prevent persistent functional issues. A thorough evaluation before any procedure helps ensure that a release is indicated and that benefits outweigh potential risks. Open communication and scheduled follow-up allow clinicians to address complications early if they occur.
Some infants show immediate improvements in latch and feeding mechanics after a successful release, while others improve more gradually as they relearn efficient movement patterns. Immediate changes are common when physical restriction was the primary barrier, but babies who have compensated for restricted motion may require days to weeks of coordinated feeding support to consolidate gains. Speech changes, when relevant, tend to be later-developing and may require evaluation by a speech-language pathologist for targeted therapy.
Follow-up appointments help the care team document progress and adjust therapy or exercises as needed, and outcomes are generally favorable when a release is part of a coordinated plan that includes feeding support. Parents should expect a variable timeline and be prepared to engage in recommended aftercare and therapy to optimize results. Ongoing collaboration among the clinician, pediatrician, and therapists ensures a consistent approach to recovery and development.
Coordinated care brings together different perspectives to identify the true cause of feeding or speech problems and to design a unified plan that addresses each contributing factor. Pediatricians provide medical oversight, lactation consultants assess and optimize feeding technique, and speech or feeding therapists support functional rehabilitation after a release. This multidisciplinary approach reduces the risk of unnecessary procedures and improves the likelihood of a successful, durable outcome.
At Happy Campers Pediatric Dentistry the team emphasizes partnership with outside professionals to ensure consistent messaging and follow-through for families, and complimentary consultations include discussions about when collaborative care is warranted. When everyone involved understands the goals and the steps required for recovery, families benefit from clearer expectations and better coordinated follow-up. Open communication channels make it easier to tailor interventions and measure progress over time.
Choose a provider who centers evaluation on function, listens to your concerns, and explains the rationale for monitoring, therapy, or release in plain terms so you can make an informed decision. Look for clinicians who work with pediatricians, lactation consultants, and therapists and who offer clear postprocedure plans that include follow-up and feeding support. Experience with infant anatomy and minimally invasive techniques, plus a child-friendly, team-based approach, are important factors to consider.
During a consultation ask about the assessment process, what conservative measures will be tried first, details of the chosen technique, and the expected aftercare routine to prevent reattachment. A transparent discussion about risks, benefits, and realistic timelines helps families select the approach that best fits their child’s needs. If you would like a consultation to discuss evaluation and treatment options, contact the office to schedule a visit and learn more about the recommended next steps.
Quick Links